An EP study may be recommended to distinguish between WPW syndrome and WPW pattern. An event recorder is typically worn for up to 30 days or until you have an arrhythmia or symptoms. This wearable ECG device is used to detect infrequent arrhythmias. This portable ECG device is worn for a day or more to record the heart's rate and rhythm during daily activities. A health care provider can look for patterns among the heart signals that suggest an extra electrical pathway in the heart. Wires connect the electrodes to a computer, which displays the test results. Sticky patches (electrodes) are placed on the chest and sometimes the arms and legs. This quick and painless test measures the electrical activity of the heart. The electrocardiographic features of preexcitation were first correlated with anatomic evidence of anomalous conducting tissue or bypass tracts in 1943.If you have a fast heartbeat, your health care provider will likely recommend tests to check for WPW syndrome, such as: This phenomenon was subsequently named as Wolff-Parkinson-White (WPW) syndrome. Paul Dudley White published a case series consisting of 11 patients who experienced paroxysmal tachycardia associated with an underlying ECG pattern of sinus rhythm with short PR and bundle branch block/wide QRS. 
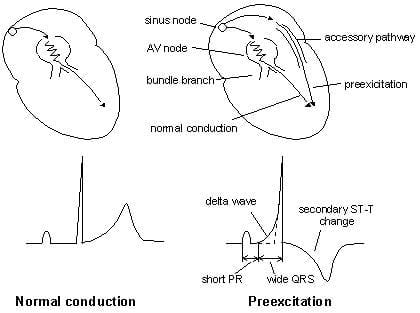
In the early 1900s, Frank Wilson and Alfred Wedd are thought to have first described ECG patterns that would later be recognized as a WPW pattern. In 1930, Louis Wolff, Sir John Parkinson, and Dr. These are referred to as concealed bypass tracts. Some accessory pathways will not manifest the described typical ECG findings, and as a result, some patients can develop a tachyarrhythmia with no prior ECG evidence that the pathway exists. Most patients with WPW pattern will never develop arrhythmia and will remain asymptomatic. The ECG findings of the WPW pattern are caused by the fusion of ventricular preexcitation through the accessory pathway and normal electrical conduction. In some settings, this pathway can result in the transmission of abnormal electrical impulses leading to malignant tachyarrhythmias. Patients with WPW syndrome have an accessory pathway that violates the electrical isolation of the atria and ventricles, which can allow electrical impulses to bypass the AV node. The action potential is delayed in the AV node and is then quickly transmitted through the His-Purkinje system to the ventricular myocytes allowing for rapid ventricular depolarization and synchronized contraction. The cardiac electrical potential originates from the sinoatrial node of the right atrium and propagates through the atria to the atrioventricular (AV) node. These units are connected by a conduction system that allows for normal cardiac synchrony and function. The normal heart consists of two electrically insulated units, the atria and the ventricles. Wolff-Parkinson-White (WPW) syndrome is a congenital cardiac preexcitation syndrome that arises from abnormal cardiac electrical conduction through an accessory pathway that can result in symptomatic and life-threatening arrhythmias. The hallmark electrocardiographic (ECG) finding of WPW pattern or preexcitation consists of a short PR interval and prolonged QRS with an initial slurring upstroke (“delta” wave) in the presence of sinus rhythm. The term WPW syndrome is reserved for an ECG pattern consistent with the above-described findings along with the coexistence of a tachyarrhythmia and clinical symptoms of tachycardia such as palpitations, episodic lightheadedness, presyncope, syncope, or even cardiac arrest.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
